Journal of Medical Case Reports volume 15, Article number: 219 (2021)
Abstract
Background
Coronavirus disease 2019 (COVID-19) is a global pandemic. The disease, typically characterized by bilateral pulmonary infiltrates and profound elevation of inflammatory markers, can range in severity from mild or asymptomatic illness to a lethal cytokine storm and respiratory failure. A number of recognized complications of COVID-19 infection are described in the literature. Common neurological complications include headache and anosmia. Guillain-Barré syndrome (GBS) is an uncommon complication described in isolated case reports. However, a causal relationship has yet to be established. This case report adds to the growing body of evidence that GBS is a potential COVID-19 complication.
Case presentation
A 70-year-old Caucasian woman with recently diagnosed COVID-19 infection presented to the emergency department with 4 days of gradually worsening ascending lower extremity weakness. Exam revealed bilateral lower extremity weakness, mute reflexes, and sensory loss. Soon after starting intravenous administration of immunoglobulin (IVIG), the patient developed respiratory distress, eventually requiring intubation. She remained intubated for the duration of her IVIG treatment. After five rounds of treatment, the patient was successfully extubated and transferred to acute rehab. Following 4 weeks of intense physical therapy, she was able to walk with assistance on room air.
Conclusion
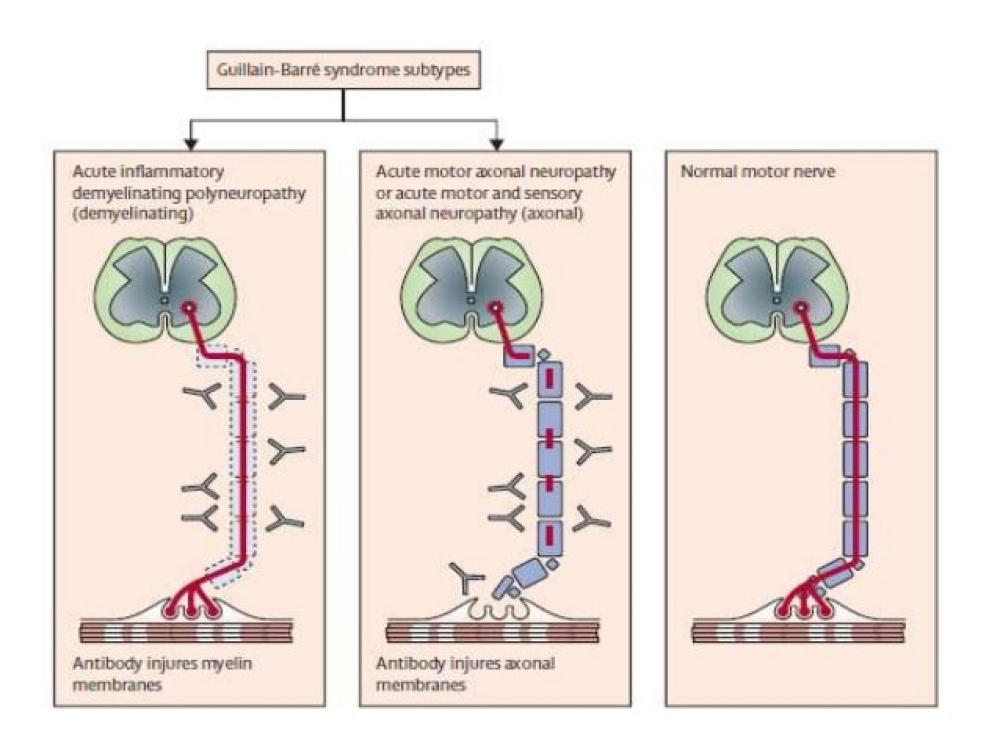
At the present time, this is one of the few reports of acute inflammatory demyelinating polyneuropathy (AIDP) or GBS associated with COVID-19 in the United States. It is unclear whether a causal relationship exists given the nature of the syndrome. However, in light of the growing number of reported cases, physicians should be aware of this possible complication when evaluating COVID-19 patients.
For More Information: https://jmedicalcasereports.biomedcentral.com/articles/10.1186/s13256-021-02831-4